
Last updated on August 4th, 2024 at 05:45 pm
Joining forces to tackle facial pain
Pain is your body’s way of telling you that something might be wrong and is the most frequent reason people seek medical care.
Facial and oral pain (in the face, mouth, and jaw) can be a symptom of injury, illness, or infection. It is one of the most common causes of pain complaints after neck, back, and knee pain.
Researchers at the National Institute of Dental and Craniofacial Research (NIDCR) wanted to explore new ways to treat facial pain without unwanted side effects. Two research teams joined forces to learn how nerves in the face send and receive information about pain. One team studies the biology of sensations such as pain, and the other has expertise in cell imaging.
Caught on camera
Ashok B. Kulkarni, Ph.D., has spent years studying a protein called cyclin-dependent kinase 5 (Cdk5). Cdk5 is involved in pain signaling in other parts of the body, and Dr. Kulkarni and his team wanted to understand its role in facial pain.
To find out, they took mice and exposed parts of their faces to different kinds of stimuli: gentle brushing, poking, heat, and chili extract.
A burn, cut, or other painful stimuli like spicy food activates receptors on the skin’s nerve endings. This triggers an influx of calcium, which acts as a message to the brain. The technique they used, called “fluorescence microscopy,” allowed the research team to watch this happen in real time as the individual cells in the mice’s facial nerves responded to each of the stimuli.
“You see calcium go up and that [looks like] a flash of light,” explained Kenneth M. Yamada, M.D., Ph.D., an NIH Distinguished Investigator. Dr. Yamada, who is Chief of the NIDCR Cell Biology Section, has expertise in developmental biology.
Protein increases sensitivity to painful and nonpainful stimuli
Under the microscope, the team saw that mice who had high levels of Cdk5 showed larger calcium surges, indicating that their pain responses were intensified. Not only that, but they were also more sensitive to all stimuli, not just the painful ones. The nerve cells responded the same way to light brushing as they did to heat and chili extract.
Dr. Yamada explained that this heightened pain sensitivity is similar to a condition called allodynia. Allodynia causes pain in response to something that isn’t typically painful (such as light touch). The research team was able to reduce pain signaling in those oversensitive mice by blocking their Cdk5.
Implications
Most pain medications work by interrupting pain signals between the brain and the body or by changing how our brains interpret those signals. These drugs can cause serious side effects because they act on multiple tissues and organs in the body. For example, narcotic drugs like opioids attach to certain receptors in brain cells. These block feelings of pain and increase feelings of pleasure, which can lead to dependence.
A drug that acts directly on the sensory neurons in the face rather than by suppressing pain signaling in the brain could offer a more direct, effective, and safer way to treat facial pain, Dr. Yamada said.
But Dr. Kulkarni explained that there’s still a long way to go before scientists can start thinking about researching these techniques in larger animals and eventually in humans. They’ll first need to identify additional compounds that act directly on Cdk5 and could be used therapeutically. One of the collaborators on the team is currently analyzing promising options. Eventually, these efforts could lead to new, safer treatments for facial pain.
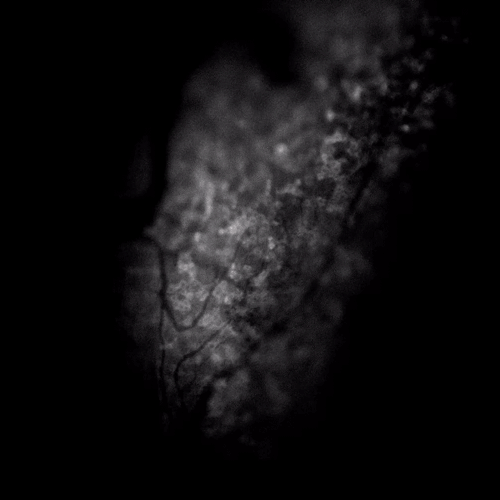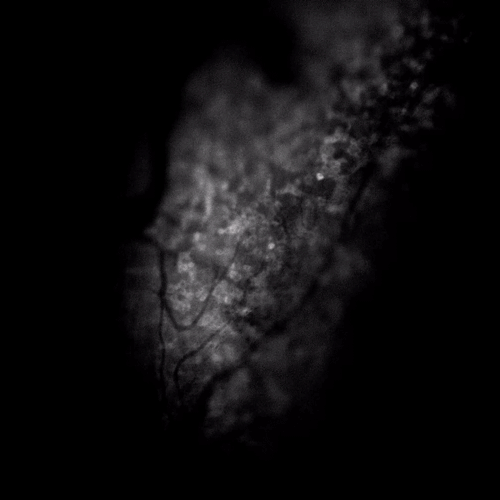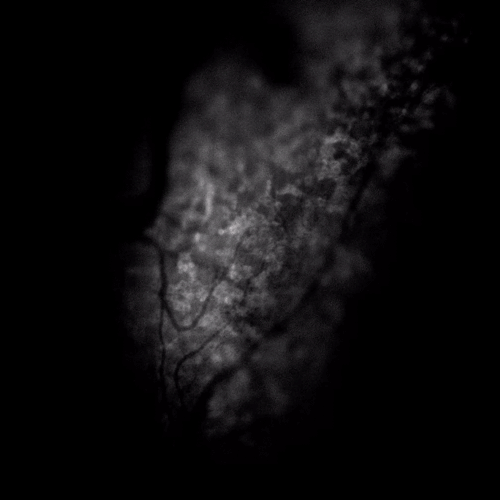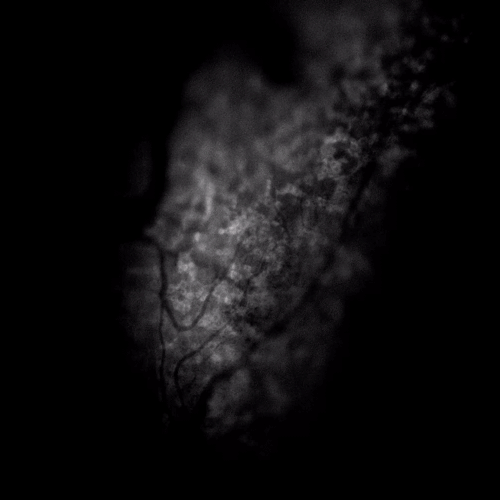
NIDCR scientists used fluorescence microscopy to visualize pain signaling in mice’s facial nerves. Here, the flickers show how calcium surges in response to a painful stimulus.
